She Was Always a Mother
“Before I ever held them, I was already fighting for them. I just didn’t know their names yet.”
Some little girls dream of becoming doctors, astronauts, or queens. I dreamed of becoming a mother. I would watch movies, mimic the labor scenes, press my hands to my belly, and pretend. I wanted the whole thing — the chaos, the exhaustion, the unconditional love that swallows you whole. Motherhood was never something I grew into wanting. It was something I was born knowing.
What I didn’t know as that little girl play-acting in her bedroom was how much it was going to cost me to get there. Not in money. In body. In blood. In faith. In grief I didn’t have words for yet.
The War Inside My Body
By the time I was 25 years old, my body was already at war with itself. Endometriosis — a disease with no cure, no clean answers, and very little mercy — had quietly been dismantling the very organs I believed I would one day use to bring my children into the world. I underwent surgery after surgery. I sat in doctors’ offices where I was handed more fear than hope. One physician looked me in the eyes after my third procedure and told me plainly: a hysterectomy was likely in my future. That the chances of me carrying a child were next to none.
I had a left ovary so ravaged by endometriosis that it was attached to my colon. My fallopian tube was crumpled and destroyed. That ovary was removed. And I grieved it the way you grieve something that held a dream inside it.
About Endometriosis: Endometriosis affects approximately 1 in 10 women of reproductive age — yet it remains one of the most under-diagnosed and under-treated conditions in women’s health. Tissue similar to the uterine lining grows outside the uterus, causing chronic pain, inflammation, and in many cases, significant damage to reproductive organs. There is currently no cure. Treatment options — including surgery, hormone therapy, and in severe cases, hysterectomy — can manage symptoms, but the disease has a well-documented history of returning. Women with endometriosis deserve to be heard, believed, and treated with the urgency their suffering demands.
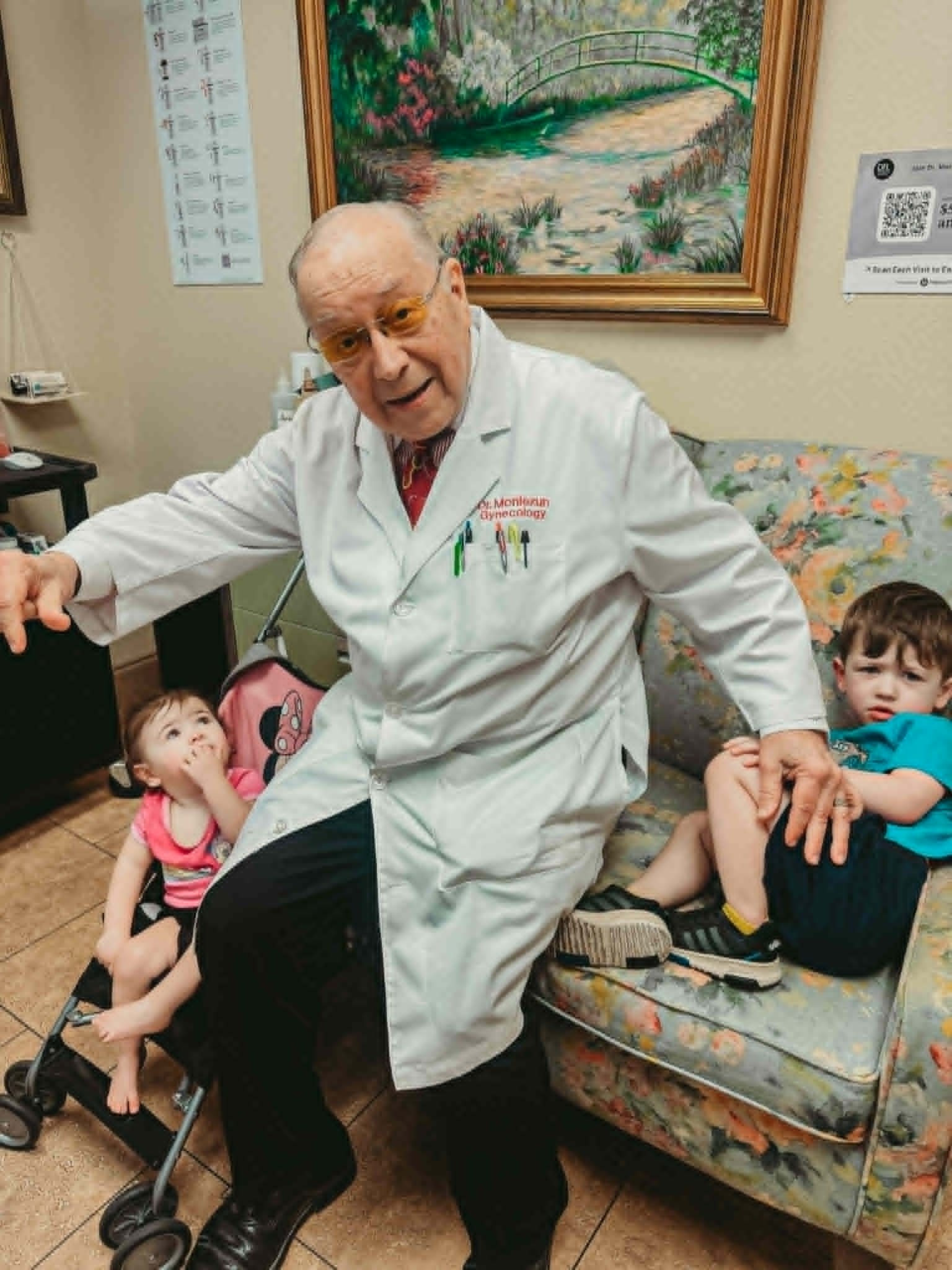
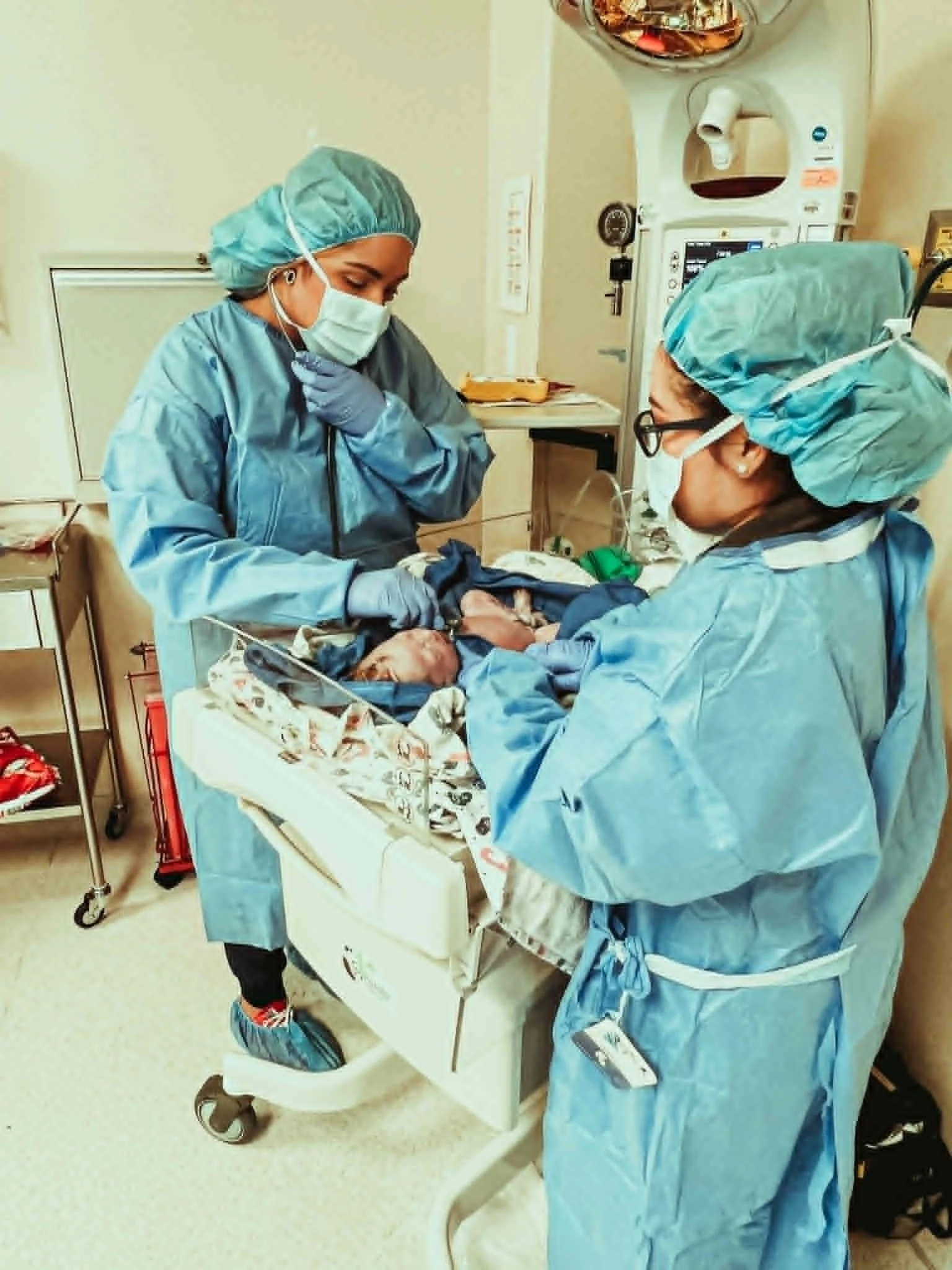
Dr. Lee Monlezun Jr. with my babies he helped me have. Forever grateful.
It was Dr. Lee Monlezun Jr. who changed the course of my story. Using a CO₂ laser — a more precise technique than standard laparoscopic surgery — he removed what he could and left me with one healthy right ovary. That ovary became my last biological frontier. And what it eventually gave me, I will never be able to fully put into words.
August 2021
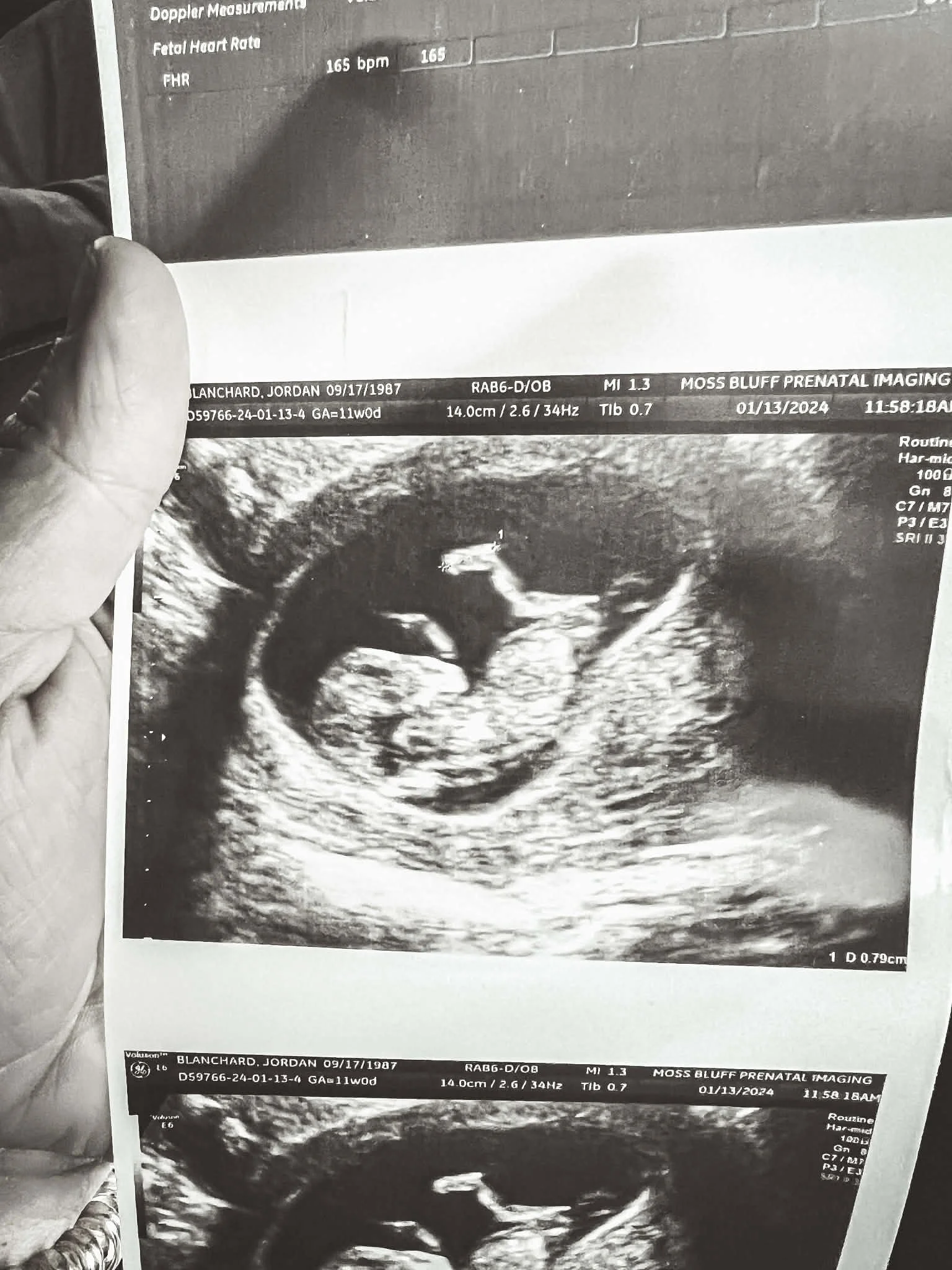
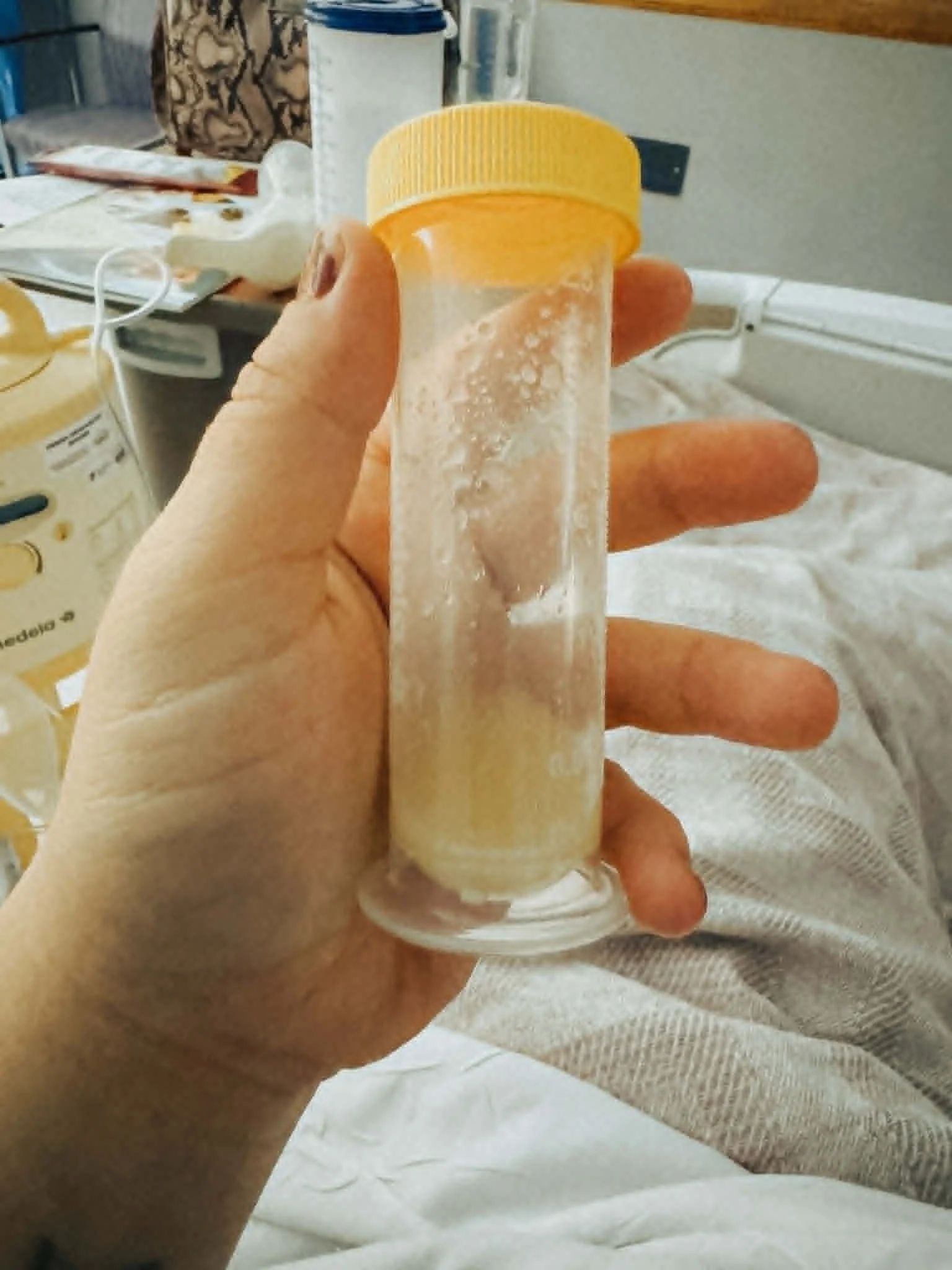
I had been tracking my ovulation for years — a quiet ritual of hope I performed with the kind of discipline that only someone who has been told “probably not” too many times can understand. I was in the bathtub when I accidentally grabbed a pregnancy test instead of an ovulation test. When I looked down and saw that dark, unmistakable line — and noticed the pink packaging instead of purple — I jumped out of that bathtub like the floor was on fire.
I ran into the bedroom. I was crying before I could even form a sentence. This has to be a joke. This can’t be real. But it was. It was real. And I fell to my knees and thanked Jesus — because that’s all I knew how to do in that moment. Not celebrate yet. Not plan. Just say thank you.
I had been trying since I was 25 years old. I was now 33. That dark line on a pink test was the answer to eight years of prayers.
Seven weeks later, I started spotting. I rushed to the emergency room, terrified. The ultrasound showed nothing. A cold, detached doctor told me I had likely miscarried and sent me home without so much as a follow-up recommendation. I cried the entire weekend. My soul felt hollowed out. Motherhood had been dangled in front of me and snatched away — and no one in that ER seemed to understand that this wasn’t just a pregnancy. It was everything I had ever asked for.
But my hCG levels wouldn’t drop. That dark line wouldn’t fade. Something told me something was still there — so I called Dr. Monlezun’s office. I went in alone. I laid on that table expecting the worst. And when the nurse placed the ultrasound wand and I saw it — a heartbeat — I completely fell apart. In the very best way. I called my husband immediately. Then I drove to that emergency room and let them know exactly how their coldness had failed me.
Loss
A week before my birthday, the bleeding came back. Bright red. Heavy. Real. I didn’t go back to the hospital that had failed me — I went to Leesville, where a doctor on call happened to be a man who had walked this exact road beside his own wife. He had me undergo another ultrasound. When the wand was removed, there was blood. I knew. the ultrasound tech knew. We didn’t need words.
The doctor sat with me in that ER room and told me about his journey. He told me that loss often happens because something wasn’t chemically right — that it was the body protecting both of us. He was kind in a way I hadn’t expected. I will never forget him. His name was Michael Johnson.
What followed was one of the most physically and emotionally traumatic experiences of my life. I still had remaining pregnancy tissue, which meant I had to take misoprostol — a medication given to complete a miscarriage. I was told it would feel like period cramps. What I experienced was a level of pain I have never ranked higher on any scale since. I laid on my bathroom floor for what felt like hours, crying out to God, in agony that was as much spiritual as it was physical. I was losing pieces of a baby I had already loved with my whole body.
“When they ask me to rate my pain from one to ten in any hospital, that day is always my ten. It always will be.”
March 2022 · My Rainbow Baby
By March 2022, we had done everything. Jeff had undergone testing and we had nearly signed up for IVF. And then — quietly, without fanfare, on an ordinary day — the test was dark again. Positive. Real.
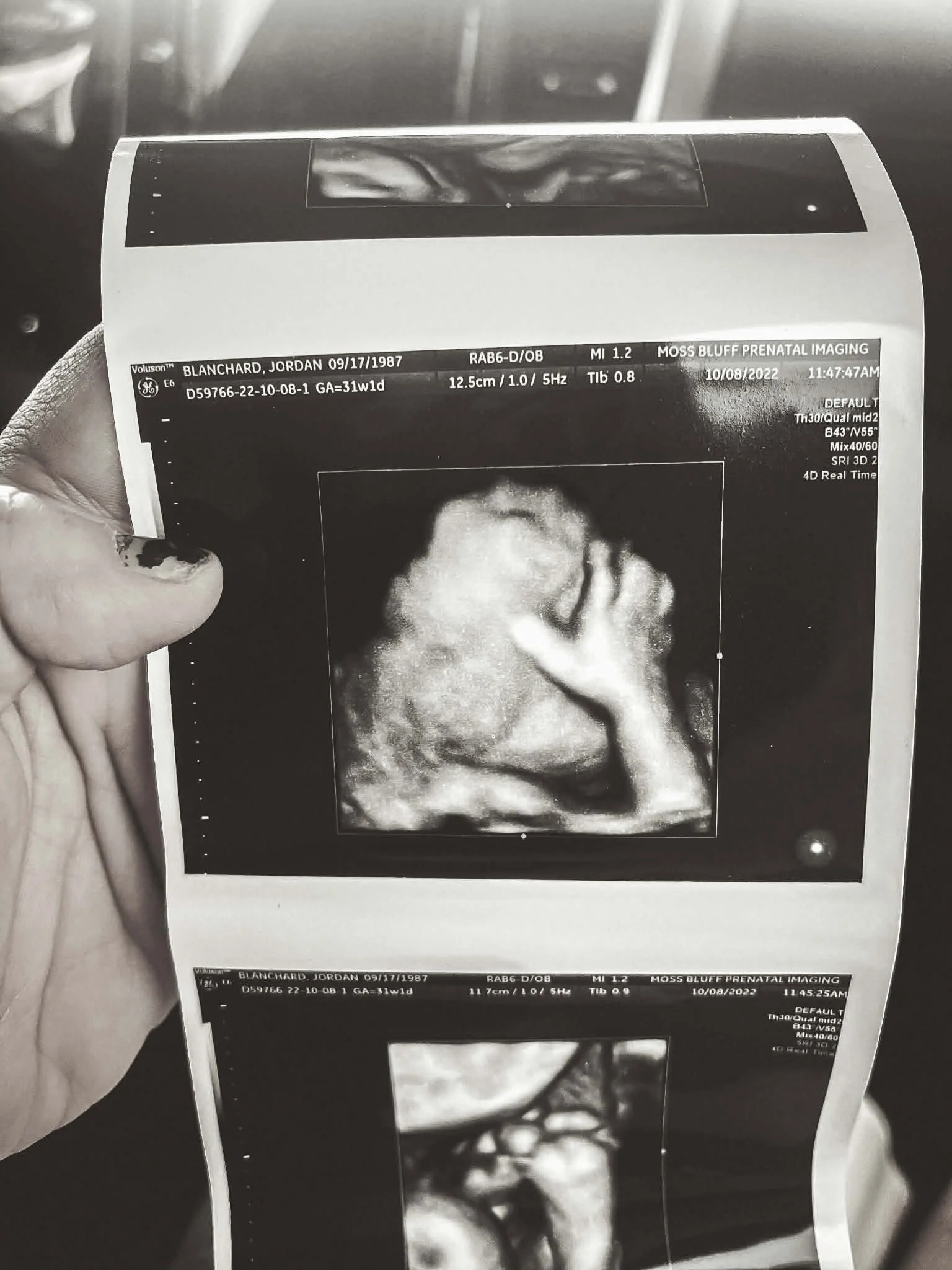
This time, joy and terror arrived together. I took a pregnancy test every single day to watch those lines. I was a woman who had already buried hope once. I wasn’t going to look away for a second. Through borderline gestational diabetes, extreme swelling, dangerously high blood pressure, and a body that fought me at every trimester — I carried him.
On November 18, 2022, Marcus entered the world via emergency C-section at 37 weeks. My blood pressure had spiked. His practice breaths were absent on ultrasound. The doctors moved fast. My epidural was administered too high in my spine and I felt completely paralyzed — panicked, certain I was dying on that table while no one would listen to me. They sedated me. I woke up groggy and overwhelmed — but he was here. 7 pounds, 9 ounces of answered prayer. My boy. My firstborn. My rainbow baby.
I took that baby in my arms and made him a promise — that every day, in any way, I would love him completely. I still stand by that today.
And Then There Was Autumn
I knew I wanted to try again quickly. My body had already told me it wasn’t built for easy, and time was never on my side. After more losses — including one where I was too afraid to even test because I had already been through so much — a dark positive appeared again. I was terrified. I was also certain.
Autumn’s pregnancy was harder. My blood pressure was worse. The gestational diabetes risk was higher. At 35 weeks, sitting at work, I felt the familiar alarm in my body — something was wrong. I checked my blood pressure. It wouldn’t come down. We dropped Marcus with my parents and drove to Lake Charles.
The next morning, the ultrasound showed that Autumn wasn’t taking her practice breaths. Her heart rate was alarming. She was far smaller than expected. The decision was made. She had to come out.
I was taken back to the OR alone. I begged the anesthesiologist to get the epidural right this time. He did. But the room felt different — colder, quieter, heavy with worry instead of joy.
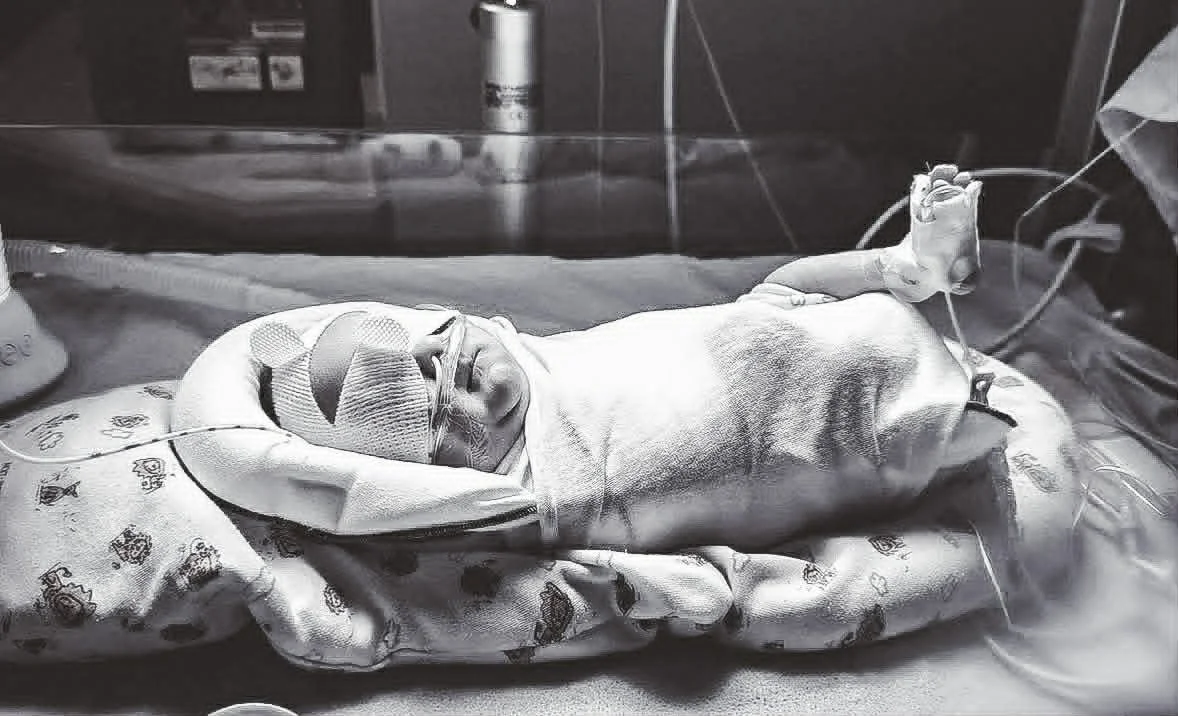
Autumn did not come out easily. It took two doctors to get her from beneath my ribs where she had been tucked safely. When she arrived, she didn’t breathe right away. They didn’t place her on my chest. They took her straight to the NICU, and I was wheeled back to my room not knowing whether my daughter was going to make it through the night.
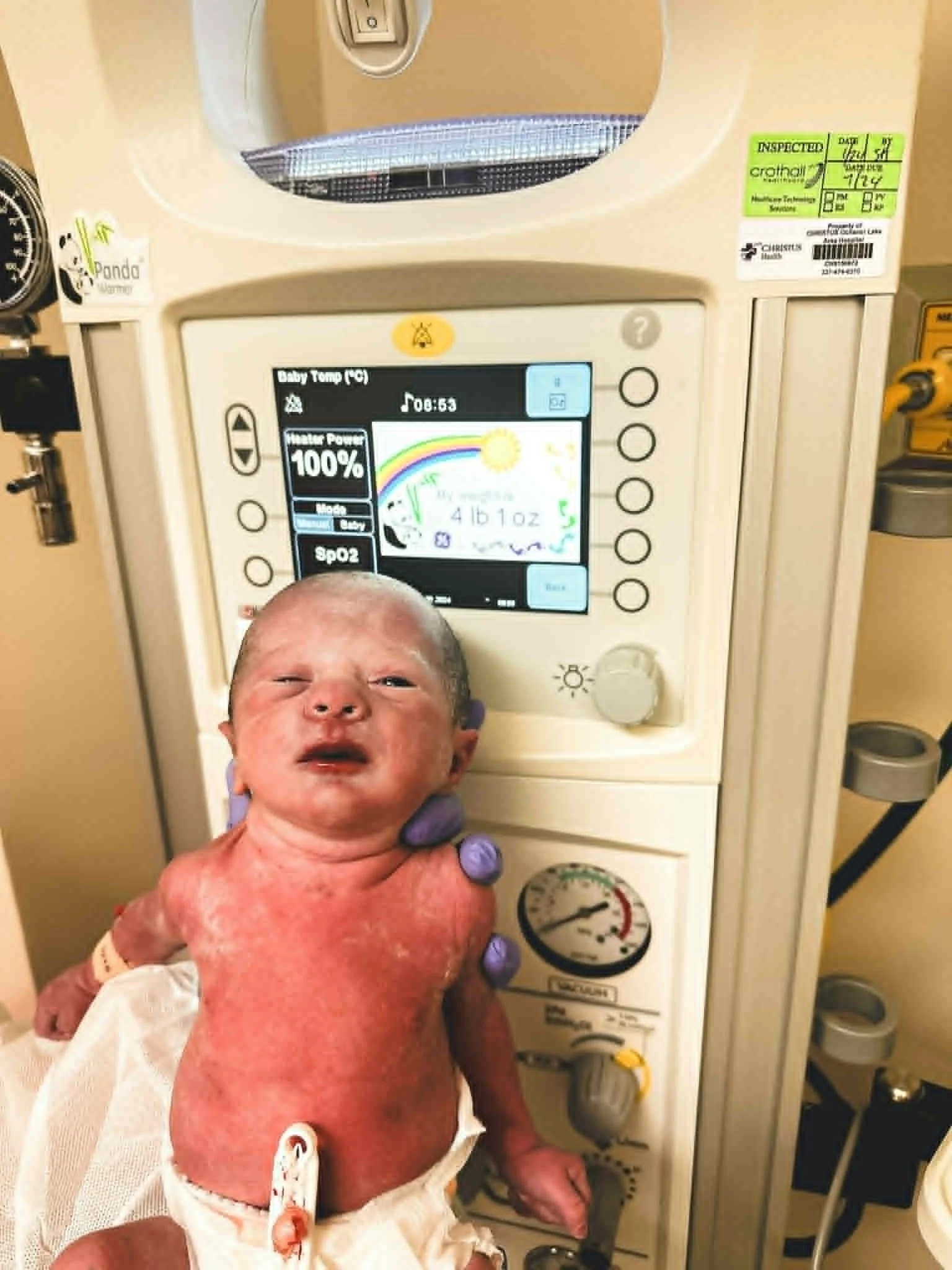
She was born at 4 pounds. She dropped to 3 pounds, 7 ounces in the NICU. And then — because she is entirely her mother’s daughter — she decided she was done. Within three days, she was breathing on her own, eating on her own, and crying so loudly that the NICU nurses nicknamed her the Banshee Queen.
My daughter came into this world at 3 pounds and 7 ounces, already fighting with everything she had. She didn’t get that from nowhere.
On June 29, 2024, we brought Autumn home in a car seat she barely fit in. I didn’t get the gallery of birth photos I had with Marcus. I didn’t get the golden hour. I had to prop my own camera up to document the first time I held her, cords and breathing monitors and all. But I have that video. And I watch it when I need to remember what strong looks like.
The Hardest Chapter
In 2025, the pain I had known since I was 25 years old came back. Different location. Same familiar feeling I had learned to recognize. Dr. Monlezun — who no longer performs surgery but will always be the man who gave me my reproductive life back — referred me to Dr. James Brown in Lake Charles. After reviewing everything I had been through, the recommendation was clear: hysterectomy.
I wanted six children. At minimum, three. And a man in a white coat was telling me that the door to that dream needed to close — because if it didn’t, the next pregnancy could kill me. Could kill us both.
I sat in that office and the room went silent. Not the peaceful kind. The kind that rings.
In July 2025, I had the hysterectomy. I went into that operating room with my father in the waiting room, my husband at his job, my babies at daycare. On the table, I said goodbye — not out loud, but internally. To organs that had caused me years of pain but had also, somehow, miraculously, helped me build my entire world. I thanked them. And then I closed my eyes.
The pain didn’t fully resolve. By April 2026, I was back in surgery with Dr. Brown — this time to remove my remaining right ovary, relieve adhesions, and address endometriosis that had spread to new locations, including an area called the cul-de-sac of the vagina. That ovary — the one that carried me through two pregnancies, the one that felt like the last piece of me that was still biologically mine — is now gone too.
Endometriosis does not always end with a hysterectomy. There is no cure — only management, adaptation, and continuing to fight in a body that doesn’t always cooperate. If this is your story too, know that you are not failing. You are surviving something most people will never understand.
Why I Do What I Do
I photograph mothers because I know what it costs to become one. I know what it feels like to lie on a bathroom floor in pain and wonder if any of it will ever be worth it. I know what it feels like to hear a heartbeat for the first time and shatter open from the inside out. I know what it feels like to not get the birth photos, to not get the golden hour, to not get the experience you dreamed of — and to love your child so fiercely anyway that none of it matters and all of it matters at the same time.
When I pick up my camera and point it at a mother, I am not just documenting a moment. I am saying: your story matters. You matter. This — all of this — deserves to be preserved.
The Matriarch Effect exists because I believe the women who carry the most — who endure, who lose, who rebuild, who show up every single day — are the ones whose stories get told the least. I want to change that. One frame at a time.
“You are not alone in your pain. I am right here — still fighting, still grateful, still yours.”
— Jordan Blanchard, The Matriarch Effect Photography